电解质异常病患之常规检查.docx
《电解质异常病患之常规检查.docx》由会员分享,可在线阅读,更多相关《电解质异常病患之常规检查.docx(11页珍藏版)》请在冰点文库上搜索。
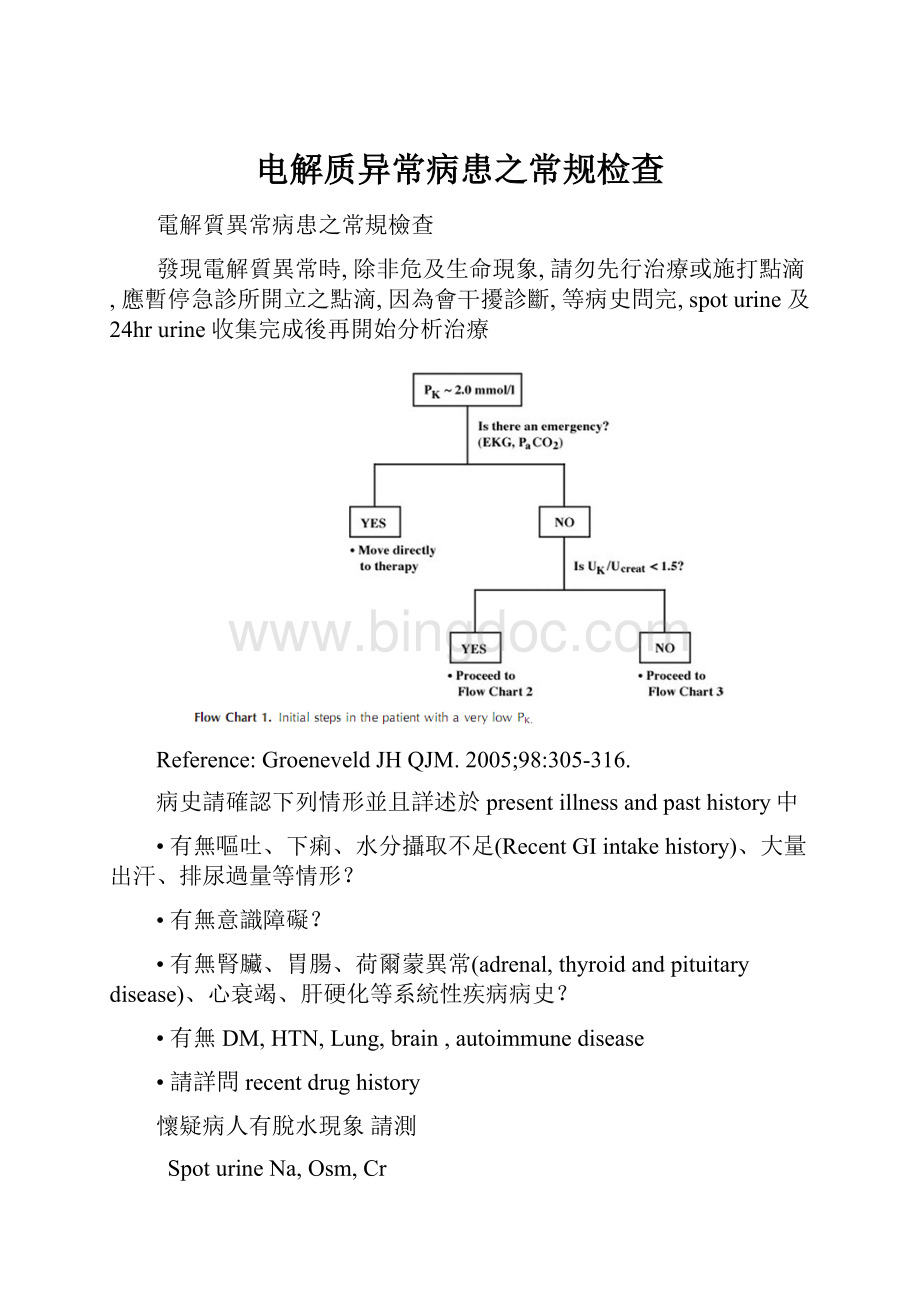
电解质异常病患之常规检查
電解質異常病患之常規檢查
發現電解質異常時,除非危及生命現象,請勿先行治療或施打點滴,應暫停急診所開立之點滴,因為會干擾診斷,等病史問完,spoturine及24hrurine收集完成後再開始分析治療
Reference:
GroeneveldJHQJM.2005;98:
305-316.
病史請確認下列情形並且詳述於presentillnessandpasthistory中
•有無嘔吐、下痢、水分攝取不足(RecentGIintakehistory)、大量出汗、排尿過量等情形?
•有無意識障礙?
•有無腎臟、胃腸、荷爾蒙異常(adrenal,thyroidandpituitarydisease)、心衰竭、肝硬化等系統性疾病病史?
•有無DM,HTN,Lung,brain,autoimmunedisease
•請詳問recentdrughistory
懷疑病人有脫水現象請測
SpoturineNa,Osm,Cr
Blood:
CBC(HCT),BUN/Cr,Osm,Na
FeNa
Urineamount
PE:
skinturger,tongue,axillarymoisture,三態血壓,pulserate
治療Order請開
Bodyweightqd
Urineamountqd
Abdominalecho(19001X,放射科執行;看腎臟有無異常如nephrocalcinosis)
Blood請check:
Na,K,Cl,Mg,Ca,Uricacid,P,
BUN,Cr,Glu,HgB
Alb,Totalprotein,Osm,
ABG(包含pH,HCO3)
Renin,cortisol,aldosterone,thyroidfunction
SpotUrine(應在急診入院後且治療前,盡快完成檢查)
Na,K,Cr,Osm,Ca,urineacid,P,Cl,Mg
UrineABG:
目的要算△(U-B)PCO2(normal>20),檢查distaltubule是否正常
24hrUrine(Spoturine收完馬上囑主護開始收24hrurine,不要等到次日再開始)Na,K,Cr,Osm,Ca,urineacid,P,Cl,Mg
於病歷上記載上述所有檢查結果.並且計載下列計算結果
Fe(Na,Ca,uricacid,Mg,P,HCO3)
(U/P)Na
例如FeNa=--------------------x100%
(U/P)Cr
(U/P)K
TTKG=----------------------------
(U/P)Osm
UK,UCr(使用spoturine結果計算即可)
Bloodaniongap=Na–Cl–HCO3
Urineaniongap=Na+K–Cl(使用spoturine計算即可)
Calculatedosm;Osmolalitygap
若懷疑pituitaryfunction異常,請測
TSH,ACTH,LH/FSH,GH,PRL,ADH
PituitaryMRI
Gonadfunction也要一起測,17-estradiol,testosterone
相關教科書資料表格或本講義有關流程圖請列印貼病歷供查房時討論
最後請先思考疾病可能原因,再與主治醫師討論
若為鉀離子疾病,請練習快速診斷法:
使用spoturineK/Cr,TTKG以及EKG,在24hrsurine尚未收集前就快速診斷到底低血鉀是因intracellularshift或Kdeficit(loss)
SpotUrineK/Cr:
IntracellularshiftlargeKdeficit
Reference:
LinSH,ArchInternMed,2004;164,1561-1566
PS:
請注意urineK與serumCr單位,需先換算為mmol
SerumCr1mg/dl=88μmol/L=0.088mmol/L
若懷疑是Thyroitoxicosis,請務必檢視EKG:
Relativelyrapidheartrate,highQRSvoltage,andfirst-degreeAVblockareimportantcluessuggestingTPPinpatientswhopresentwithhypokalemiaandparalysis.Hsuetal.Electrocardiographicmanifestationsinpatientswiththyrotoxicperiodicparalysis.AmJMedSci.2003;326:
128-32
Reference:
GroeneveldJHQJM.2005;98:
305-316.
Reference:
GroeneveldJHQJM.2005;98:
305-316.
Dedinitions
Hypokalemicperiodicparalysis(HPP):
shiftofKintocells,(有4個elements)
1.Positivefamilyhistory,clinicallyrecurrent,hyperthyroidism,
2.AbsenceofintakeofagentscausingintracellularKshift
3.Thepatientsrequire<1.5mmol/kgKCLtoreturntonormalK
4.Noacid-basedisorder
Non-hypokalemicperiodicparalysis(Non-HPP):
duetoalargedeficitofK
1.>3mmol/kgofKtocorrectplasmaK
2.Ifacid-basedisorderispresent
Reference:
LinSH,ArchInternMed,2004;164,1561-1566
Reference:
LinSH,ArchInternMed,2004;164,1561-1566
Reference:
LinSH,ArchInternMed,2004;164,1561-1566
LinSHCurrMedicinalChem2006
WashingtonManual32edition
Reference:
LinSH,QJMed2001;94:
133-139
Normalrange
下列三者代表proximaltubulefunction正常
FeUricacid<12%or7~12
FeP<10
FeHCO3<5%normal;>15%proximalRTA
FeMg(>3%,renalloss)
Uk/Ucr(mmol/mmol)>1.5renalloss
Uca/Ucr(mg/mg)0.1-0.2
Reninsupine3-16pg/ml
upright3-33pg/ml
Aldosterone37.5-240pg/ml
下列代表distaltubulefunction正常
△(U-B)PCO2>20
備註:
對於每一位電解質病患(especiallyrenale-loss,RTA),除了判斷出腎原性以外,請嘗試去判斷到底是proximaltubuledefectordistaltubuledefect
DailyurineNa100-260mEq/day
DailyurineK25-100mEq/day
DailyurineP400-1300mg/day
Dailyurineuricacid250-750mg/day
SIADH治療需限水,補充鹽水時只能用3%NaCl,因為normalsaline會把serumNa越打越低
Hypovolemichyponatremia治療算法(例:
以normalsaline1000cc=154meq/L來治療;公式中1代表TBW增加1liter;男生TBW=TBWx0.6;女生TBW=TBWx0.5;PNa代表血鈉;△[Na]代表經normalsaline1000cc治療後血鈉上升量)
154-PNa
△[Na]=---------------------------
TBW+1
•
Δaniongap/ΔHCO3-
Thereisa1:
1relationshipbetweentheincreaseinAG(ΔAG)andthedecreaseinplasmabicarbonate(ΔHCO3)
<1CombinedhighandnormalAGacidosiseg.Diarrheawithrenalinsufficient
1~2AnuncomplicatedhighAGmetabolicacidosis
>2Combinedmetabolicalkalosiseg.vomiting
DeltaRatio
AssessmentGuideline
<0.4
Hyperchloraemicnormalaniongapacidosis
0.4-0.8
ConsidercombinedhighAG&normalAGacidosisBUTnotethattheratioisoften<1inacidosisassociatedwithrenalfailure
1to2
Usualforuncomplicatedhigh-AGacidosis
Lacticacidosis:
averagevalue1.6
DKAmorelikelytohavearatiocloserto1duetourineketoneloss(espifpatientnotdehydrated)
>2
Suggestsapre-existingelevatedHCO3levelsoconsider:
1.aconcurrentmetabolicalkalosis,or
2.apre-existingcompensatedrespiratoryacidosis
Elevatedaldosteroneandrennin
Aldosterone/rennin>20primaryhyperaldosteronemia
Aldosterone/rennin<10secondary